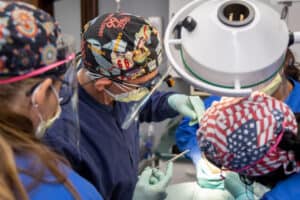
Part Of The Wisdom Tooth Removal Process
As part two of our blog on wisdom teeth removal and anesthesia, today, we’re going to talk about sedation.
The purpose of sedation is to make the patient unaware of the fact that they’re undergoing a procedure. Under sedation, the patient has no awareness of pain, pressure, or discomfort of any type. In addition, they will have no recollection of the experience afterwards, which automatically makes for a much better experience.
The agents used to sedate patients for oral surgery are the same agents used at major medical centers each day, on thousands of people undergoing all types of surgeries. Prior to beginning the procedure on a patient who has been sedated, local anesthetic will be used in order to eliminate any pain they may experience after waking from sedation. By the time the local anesthetic wears off, the patient will be home with their prescriptions.
Like wisdom teeth removal, many people think sedation is extremely dangerous.
In speaking with my patients, it seems everyone knows someone who died from “bad anesthesia.” Everyone has a cousin, a neighbor, a neighbor’s cousin, or someone they know who had some type of procedure done under sedation and never woke up. However, when people are pressed on the details of such ghastly tragedies, they can’t provide any.
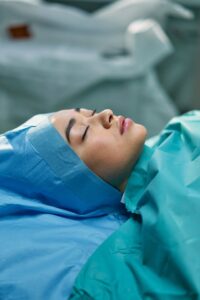 In reality, sedation does carry risks, and poor outcomes are possible; they’re just not nearly as likely as many people believe.
In reality, sedation does carry risks, and poor outcomes are possible; they’re just not nearly as likely as many people believe.
Many people will believe the worst about anything and repeat it to anyone they can. Friends or family members from other countries can perpetuate fears, since complications from medical procedures in general occur much more frequently in underdeveloped areas than they do in the US.
The truth of the matter is that in the US today, the odds of sedation itself leading to a tragic outcome are very slim, and if they weren’t, scores of surgeons would be out of business.
The very small number of people who’ve had negative experiences with sedation typically experienced them for one of two reasons: improper administration, or a pre-existing health problem that was the true culprit behind the bad outcome.
I have received the proper clinical training in the specific sedation techniques I employ, and I carefully screen each patient prior to performing surgery. I follow the same guidelines that are used in major surgical centers to evaluate each patient and ensure that he or she is a good candidate for undergoing every aspect of a procedure, sedation included.
As part of this evaluation process, I review each patient’s medical history in order to determine what medications they’re taking, what health problems they have, whether or not they drink alcohol, smoke, or use any street drugs, what types of surgeries they’ve previously undergone, and whether they or any of their family members have encountered unexpected issues or problems with anesthesia in the past. I will also check patients’ airways and ensure that their blood vessels are suitable for the intravenous lines we use.
Not everyone turns out to be a good candidate for extraction under sedation – some people have complex health issues such as poorly-controlled diabetes, severe asthma, sleep apnea, or heart disease that make the risks of surgery under sedation outweigh the benefits. In such cases, I can still remove their wisdom teeth using local anesthesia and nitrous oxide and minimize their discomfort as much as possible.
If you need your wisdom teeth removed and have questions, please contact our office for your consultation to get answers, check out the information on this site and our Facebook page.